Peripheral Arterial Disease (PAD): Evidence-Based Diagnosis, Treatment, and Safety
Peripheral Arterial Disease (PAD) is a common but often underdiagnosed vascular condition that affects blood flow to the legs. When left untreated, PAD can lead to worsening pain, non-healing wounds, limb loss, and increased risk of heart attack and stroke.
This page explains what current medical evidence shows about how PAD is diagnosed, when treatment is necessary, which therapies are supported by research, and how safety is evaluated—so patients can make informed decisions based on facts, not fear.
For a general overview of symptoms and causes, visit our Peripheral Arterial Disease (PAD) overview.
What Is Peripheral Arterial Disease?
Peripheral Arterial Disease occurs when arteries supplying the legs become narrowed or blocked, most often due to atherosclerosis. Reduced blood flow limits oxygen delivery to muscles and tissues, especially during activity.
PAD is frequently confused with other causes of leg pain, including vein disease and peripheral neuropathy. Accurate diagnosis is essential, as treatment strategies differ significantly.
Why Evidence-Based PAD Care Matters
PAD treatment is not one-size-fits-all. Some patients improve with lifestyle and medical therapy alone, while others require intervention to prevent serious complications.
Evidence-based care helps:
![]()
Avoid unnecessary procedures
![]()
Identify patients who truly benefit from intervention
![]()
Reduce the risk of limb loss and cardiovascular events
![]()
Ensure treatments are timed appropriately
This is why proper evaluation and specialist-guided decision-making are critical.
How PAD Is Diagnosed: Accuracy and Evidence
Ankle-Brachial Index (ABI) and PVR Testing
The ankle-brachial index (ABI) compares blood pressure in the ankle to the arm and is a widely used screening tool for PAD. When combined with pulse volume recordings (PVR), ABI testing provides valuable information about blood flow severity.
Learn more about how these tests work in ABI and PVR testing for PAD.
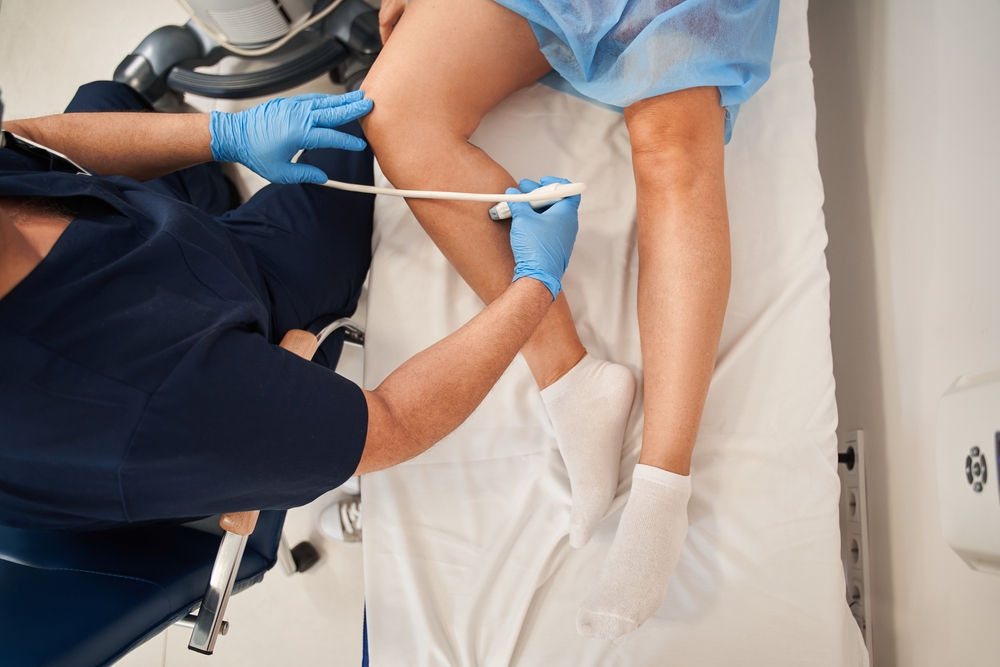
Duplex Ultrasound
Duplex ultrasound is the foundation of PAD diagnosis. It directly visualizes blood flow, identifies blockages, and measures their severity—without radiation or contrast dye.
This non-invasive test plays a central role in determining whether treatment is necessary. See how it works in duplex ultrasound evaluation.
CT vs MR Angiography
Advanced imaging such as CT angiography (CTA) or MR angiography (MRA) is used when detailed anatomical information is needed, especially before intervention.
Each modality has benefits and limitations related to kidney function, contrast use, and image clarity. A full comparison is available in CT vs MR angiography for PAD.
While ABI is reliable for many patients, results can be falsely elevated in individuals with diabetes or arterial calcification, which is why additional testing is often needed.
Evidence-Based Treatment Options for PAD
PAD treatment depends on symptoms, disease severity, and overall health risk.
Lifestyle and Medical Therapy (First-Line Treatment)
For many patients with mild PAD, conservative therapy is highly effective and supported by strong evidence.
This includes:
- Supervised exercise therapy, which improves walking distance and circulation
(see the role of exercise in PAD) - Smoking cessation to prevent further arterial damage
(see how smoking damages arteries) - Cholesterol and blood pressure control
- Antiplatelet therapy to reduce clot risk
These measures also reduce the risk of heart attack and stroke, which commonly coexist with PAD (see PAD and heart disease).
When Minimally Invasive Treatment Is Appropriate
When symptoms persist despite conservative care—or when circulation is severely impaired—minimally invasive treatment may be recommended.
 Angioplasty
Angioplasty
Angioplasty for PAD uses a small balloon to open narrowed arteries and restore blood flow. It is supported by extensive clinical evidence for improving symptoms in appropriately selected patients.
Learn more about this approach in angioplasty for PAD.
 Atherectomy
Atherectomy
Atherectomy removes plaque from inside the artery and is often used for heavily calcified disease or in combination with angioplasty.
Evidence-based indications and techniques are explained in what is atherectomy and atherectomy with angioplasty.
 Stents
Stents
Stents are used selectively when arteries do not remain open after angioplasty alone. Their use depends on anatomy, location, and disease severity.
See when they are appropriate in when stents are necessary for PAD.
Surgical Bypass: When Is It Necessary?
Surgical bypass is typically reserved for advanced PAD or cases where endovascular therapy is not effective or feasible.
This option carries higher risk but can provide durable results in selected patients. Learn more in PAD treatment vs bypass surgery and when surgery is necessary for PAD.


Safety and Potential Complications
All PAD treatments carry some risk, but evidence-based care minimizes complications.
Potential risks include:
- Bleeding or bruising
- Contrast-related kidney strain
- Re-narrowing of arteries (restenosis)
Modern minimally invasive techniques are designed to reduce these risks. Learn why experience and technology matter in minimally invasive vascular care.
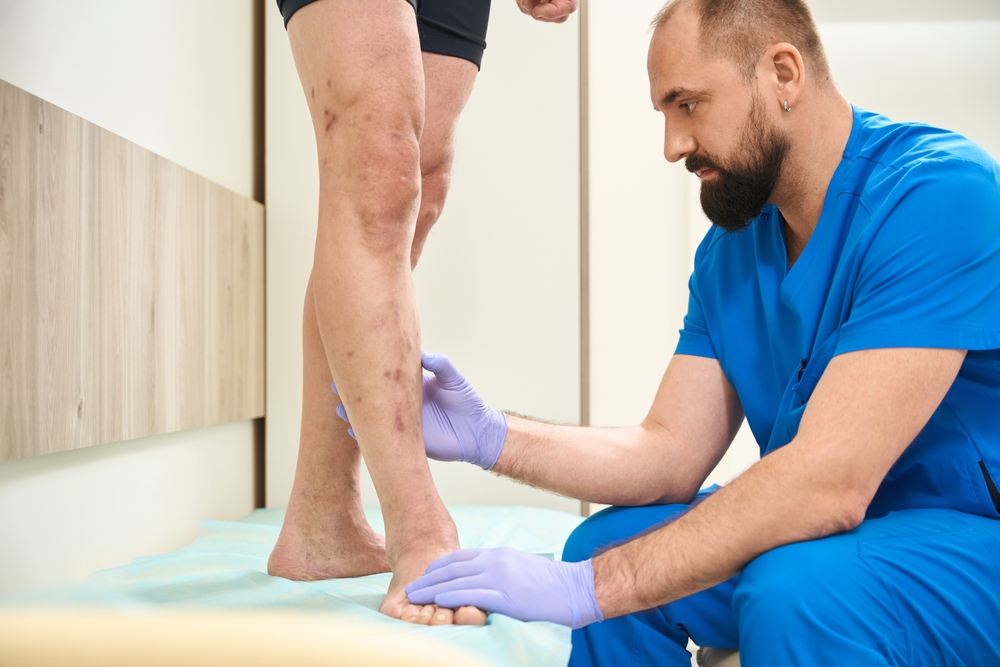
What Happens If PAD Is Left Untreated?
Untreated PAD often progresses over time. As circulation worsens, patients may develop:
- Worsening leg pain
- Non-healing wounds
- Rest pain
- Tissue loss
Advanced disease can lead to critical limb ischemia, which significantly increases the risk of amputation. Warning signs are outlined in signs of severe PAD and signs your PAD has progressed.
Early treatment improves the chance of limb salvage and reduces cardiovascular risk.
Who Benefits Most From PAD Intervention?
Evidence shows the greatest benefit from intervention in patients with:
![]()
Lifestyle-limiting claudication
![]()
Rest pain
![]()
Non-healing foot wounds
![]()
Progressive disease despite medical therapy
Not all patients require immediate intervention, which is why evaluation by a vascular specialist is essential.

Limitations of Current PAD Research
While PAD treatment is guided by strong clinical evidence, limitations remain:
- Outcomes vary by artery location and disease severity
- Restenosis can occur over time
- Long-term management is individualized
Ongoing research continues to refine best practices and improve outcomes.
- Summary: Evidence-Based PAD Care Improves Outcomes
Peripheral Arterial Disease is a serious but treatable condition. Evidence-based diagnosis and treatment reduce symptoms, prevent complications, and improve quality of life.Early detection, appropriate testing, and individualized care decisions are key to achieving the best outcomes.For a general overview, visit Peripheral Arterial Disease (PAD).
- Medical Review & References
This page reflects current clinical evidence and guideline-based care for PAD, including diagnostic standards and treatment recommendations from vascular societies and cardiovascular research organizations.
Schedule a Consultation at Our Manhattan Vein Treatment Center
If you’re looking for a vein specialist near you or a trusted vein treatment center in Manhattan, NY, Fox Vein Care is here to help. Schedule your vein consultation today and take the first step toward healthier legs.
We Accept Most Insurances
We work with most major insurance providers. Contact us to confirm coverage.
