It usually starts with a random ache after a long walk or a bit of stiffness when you get out of bed. For a long time, you might just brush it off as normal aging or a minor tweak. But as the weeks and months pass, the discomfort becomes harder to ignore.
Most patients find themselves dealing with this exact uncertainty. You start to wonder if that occasional twinge is just wear and tear, or if it is the beginning of something more serious. If you have been dealing with persistent knee pain, you are probably trying to figure out exactly what is happening inside your joint.
Understanding the stages of knee osteoarthritis is critical because it helps you make informed decisions about your health. People rarely search for “osteoarthritis” just out of curiosity. They search because they want to know if they are in the early stages, if they waited too long, or if they are dangerously close to needing surgery.
Knowing how knee arthritis progresses over time gives you clarity. It helps you recognize where you are in the process and, more importantly, what non-surgical treatment options are still available to help you reclaim your mobility.
Knee Arthritis Doesn’t Happen All at Once
Why osteoarthritis usually develops gradually
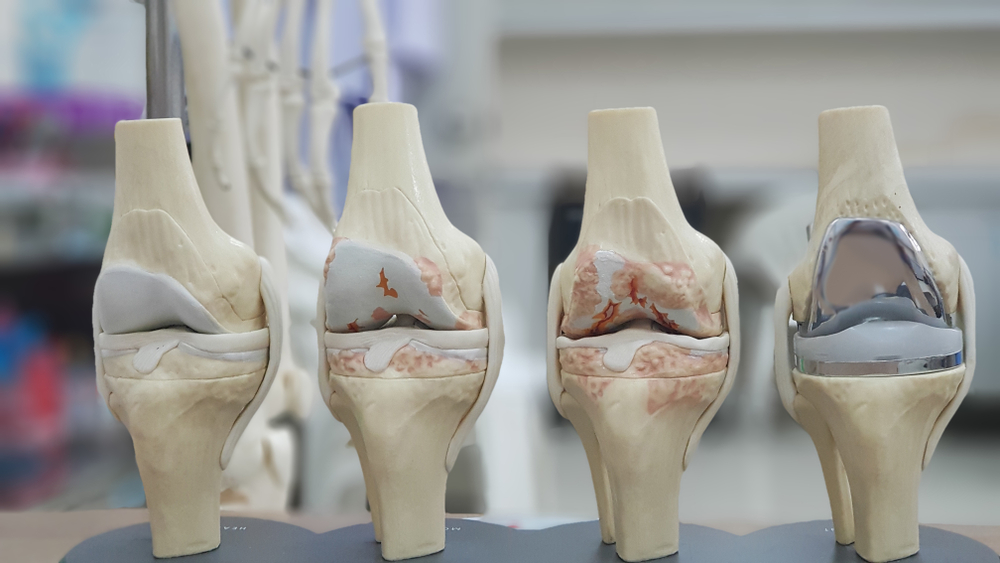
Knee osteoarthritis is not a sudden injury. It is a slow, gradual process that happens over years. The protective cartilage that cushions the ends of your bones slowly wears down. As this cartilage thins, the joint loses its natural shock absorber. Because the changes happen on a microscopic level at first, you will not wake up one day suddenly in the late stages of knee osteoarthritis. The progression sneaks up on you, often taking years before it starts interfering with your daily routine.
Why symptoms and imaging don’t always progress together
One of the most confusing parts of knee arthritis is that your pain levels do not always match your X-rays. A doctor might look at a scan and see significant cartilage loss, yet you might only feel mild discomfort. Conversely, you could be in severe agony, but your MRI only shows early stage knee arthritis. This happens because cartilage itself does not have nerve endings. The pain you feel actually comes from surrounding tissues, inflammation, and changes in the bone underneath the cartilage.
Why “stage” matters for treatment decisions
Knowing your knee arthritis stages is not just about putting a label on your condition. The stage dictates your treatment path. If you catch it early, simple lifestyle changes and physical therapy can drastically slow down the progression. If you are in the moderate stages, you might need targeted interventions to manage inflammation and pain. Understanding your stage prevents you from jumping straight to drastic surgical measures when less invasive options could still work perfectly well.
Stage 1: Early Knee Arthritis
Mild stiffness and occasional discomfort
At this point, you might not even realize you have arthritis. Stage 1 is categorized by very minor wear and tear. You might feel a little stiff when you wake up, or you might notice a dull ache after a strenuous hike or a long run. The pain is not constant. It usually goes away quickly with rest or an over-the-counter pain reliever.
Small cartilage changes that may not show obvious symptoms
Inside the joint, the cartilage is just starting to soften or develop tiny surface cracks. Your body is still doing a great job of compensating. The joint space between your bones remains normal, and your knee functions exactly as it should. If you were to get an X-ray for an unrelated issue, a doctor might spot these tiny changes, but they usually do not cause any significant mechanical problems.
Why early treatment matters more than most people realize
Because the pain is manageable, most people ignore early stage knee arthritis. This is a missed opportunity. Making small adjustments now can significantly delay the onset of moderate knee arthritis symptoms. Strengthening the muscles around your knee, maintaining a healthy weight, and staying active can protect the joint and keep the cartilage healthier for a much longer period.
Stage 2: Mild to Moderate Progression
More consistent pain with walking and stairs
As you enter stage 2, the symptoms become harder to ignore. The occasional ache turns into a more predictable pattern. You will likely feel pain when walking long distances, kneeling, or going up and down stairs. The stiffness might last a bit longer in the morning, and your knee might feel tight after sitting at a desk or in a car for a few hours.
Swelling, inflammation, and activity-related symptoms
This is the stage where inflammation really starts to show up. After a busy day on your feet, your knee might look visibly swollen or feel warm to the touch. The cartilage is now visibly thinning on imaging, and your body might start forming small bone spurs, known as osteophytes, as it tries to stabilize the joint.
When conservative treatments usually begin
Stage 2 is when most people finally make an appointment with a doctor. The pain is starting to dictate what you can and cannot do on the weekends. Treatment here usually involves a dedicated physical therapy routine, supportive bracing, and non-surgical joint pain treatments. The goal is to manage the inflammation and keep the joint moving fluidly before the cartilage wears down further.
Stage 3: Moderate to Advanced Arthritis
Daily pain that starts affecting routine life
When you reach stage 3 knee osteoarthritis, the condition is actively interfering with your daily life. The pain is no longer just tied to strenuous activity. It can hurt when you are simply walking around the grocery store or trying to get comfortable in bed at night. The cartilage is significantly damaged, and the space between the bones in your knee is noticeably narrowing.
Reduced mobility and compensating movement patterns
Because your knee hurts, you naturally start walking differently. You might develop a slight limp or lean on your other leg to take the pressure off. These compensating movement patterns can lead to secondary issues, like hip or lower back pain. You will also notice that you cannot bend or straighten your knee as far as you used to, making simple tasks like putting on socks or getting out of a low chair incredibly frustrating.
Why injections often stop working well here
For many patients, this is the stage where traditional treatments start losing their effectiveness. Cortisone shots that used to provide six months of relief might only last a few weeks. Hyaluronic acid injections might not give you the same smooth feeling they once did. The joint mechanics are changing, and the chronic inflammation is becoming much harder to control with standard conservative care.
Stage 4: Severe or End-Stage Arthritis
Bone-on-bone pain and major functional limitations
Stage 4 is commonly referred to as bone on bone knee arthritis. The cartilage is almost completely gone, leaving the bones to rub directly against each other. This causes severe, sharp pain with almost any movement. The friction damages the bone surfaces and creates intense, chronic pain that is very difficult to manage with basic medications.
Joint deformity and loss of independence
In severe knee arthritis stages, the structure of the joint begins to change. The knee might look noticeably larger, swollen, or even crooked (bow-legged or knock-kneed) due to the complete loss of joint space and the growth of large bone spurs. At this point, mobility is severely limited. Patients often need a cane or walker and may have to give up hobbies, travel, or even basic household chores.
When knee replacement enters the conversation
When you have severe knee arthritis symptoms that do not respond to conservative care, and your quality of life has plummeted, doctors will start discussing knee replacement surgery. While surgery is highly effective for end-stage arthritis, it is a major procedure with a long recovery. Many patients look for alternatives to knee replacement surgery if they are not medically cleared for the operation or simply want to avoid the operating room.
Why Pain Severity Doesn’t Always Match Your Stage
Severe pain with mild imaging findings
It is incredibly frustrating to be in severe pain, only for a doctor to look at an X-ray and say your arthritis is “mild.” This happens frequently. Cartilage loss is just one piece of the puzzle. The structures around the knee, like the joint lining (synovium), the ligaments, and the bone marrow, can be highly sensitive and trigger massive pain signals even if the joint space looks perfectly fine on a screen.
Advanced imaging changes with minimal symptoms
On the flip side, some people walk around with stage 3 or stage 4 osteoarthritis and feel completely fine. Their X-rays might look terrible, showing bone-on-bone contact and massive bone spurs. Yet, they have excellent muscle strength, good joint stability, and, most importantly, low levels of joint inflammation.
The role of inflammation and blood flow
The discrepancy between pain and imaging usually comes down to inflammation and blood flow. When the joint lining becomes irritated, your body sends extra blood vessels to the area to help heal the tissue. Instead of helping, these abnormal blood vessels create a constant loop of inflammation, swelling, and pain.
How Inflammation Changes the Picture
Why synovial inflammation can drive pain early
The synovium is a thin membrane that lines the inside of your knee joint. Its job is to produce the fluid that lubricates the cartilage. In the early and moderate stages of knee arthritis, this lining can become chronically inflamed, a condition called synovitis. Synovial inflammation is highly sensitive and is often the primary driver of the aching, throbbing pain you feel, long before the cartilage completely wears away.
How abnormal blood flow contributes to ongoing symptoms
When the knee is constantly inflamed, the body tries to repair the damage by growing new, microscopic blood vessels around the joint lining. Unfortunately, these new blood vessels bring new nerve fibers with them. This abnormal blood flow essentially “wires” the knee for chronic pain. The joint stays swollen, angry, and incredibly sensitive to even minor movements.
Why treatment should target more than cartilage loss
Because pain is largely driven by inflammation and abnormal blood flow, focusing only on cartilage loss is a mistake. You cannot regrow cartilage, but you can definitely control the inflammation and shut down the abnormal blood vessels that are keeping the joint angry. Effective treatment needs to address the root cause of the pain, not just what shows up on an X-ray.
Treatment Options by Stage of Knee Arthritis
Early-stage management and prevention
If you are in stage 1 or early stage 2, the goal is preservation. Physical therapy is your best tool. Strengthening the quadriceps and hamstrings takes the mechanical load off the knee joint. Weight management is also critical, as every extra pound of body weight puts about four pounds of extra pressure on your knees. Over-the-counter anti-inflammatories and supportive sleeves can help you stay active on bad days.
Mid-stage options before surgery becomes necessary
When you reach the moderate stages, you need more targeted relief. This is where doctors typically introduce treatments like corticosteroid injections to calm acute flare-ups, or hyaluronic acid (gel) injections to add lubrication back into the joint. You might also explore regenerative medicine options, like PRP (platelet-rich plasma), to help soothe the joint environment. The focus here is keeping you mobile and comfortable for as long as possible.
Advanced non-surgical options for persistent pain
If you are in stage 3 or early stage 4 and injections have stopped working, you are in a difficult spot. You are dealing with daily pain, but you might want to avoid a total knee replacement. In these cases, advanced non-surgical joint pain treatments become highly relevant. Medical advancements have created minimally invasive procedures that target the underlying drivers of chronic pain, buying you years of relief without the need for a scalpel.
Where Genicular Artery Embolization (GAE) Fits
Why GAE is often considered in moderate arthritis stages
Genicular Artery Embolization (GAE) is a minimally invasive procedure designed to target the abnormal blood flow that causes chronic knee inflammation. During GAE, a specialist uses a tiny catheter to block the specific microscopic arteries feeding the inflamed joint lining. By shutting off this abnormal blood supply, the inflammation drops significantly, and the pain fades. GAE is highly effective for patients in the moderate to advanced stages of osteoarthritis who have constant, localized pain and swelling.
Patients trying to avoid or delay knee replacement
GAE fits perfectly into the treatment spectrum for patients who are stuck in the gap between conservative care and surgery. If physical therapy and cortisone shots are no longer providing relief, but you are not ready for a knee replacement, GAE offers a powerful middle ground. It is an outpatient procedure with a very short recovery time, making it an excellent option for adults looking to regain their mobility without a lengthy hospital stay.
When GAE may not be the right fit
GAE is a highly effective tool, but it is not a cure-all. If you have end-stage, bone-on-bone arthritis with severe structural deformities, GAE might not provide the mechanical relief you need. It reduces inflammation, but it cannot fix a joint that is completely destroyed or locked in place. A thorough evaluation by a vascular specialist is required to see if your specific pain profile matches the criteria for the procedure.
How to Know What Stage You’re In
Symptoms, imaging, and physical evaluation
Determining your exact stage requires a combination of factors. A doctor will look at your X-rays or MRI to check the cartilage thickness and joint space. They will also perform a physical evaluation to test your range of motion, check for swelling, and see exactly where the knee hurts. Your daily symptoms provide the final piece of the puzzle, confirming how the structural changes are actually impacting your life.
Why self-diagnosing from pain alone is difficult
You cannot accurately guess your stage just by how much your knee hurts. As we discussed, severe pain can happen in early stages due to acute inflammation, while some advanced stages feel perfectly fine. Assuming you are “bone-on-bone” just because you have a bad flare-up can cause unnecessary anxiety and lead you to think surgery is your only option.
Why timing matters more than perfection
You do not need to obsess over whether you are a “late stage 2” or an “early stage 3.” The exact label matters less than the timing of your action. What stage is my knee arthritis? The answer is less important than asking what you can do about it today. Recognizing that your pain is progressing and seeking a professional evaluation early gives you the widest range of non-surgical options.
Next Step: Don’t Wait Until It Feels “Bad Enough”
Many people wait entirely too long to seek help for their knee pain. There is a common misconception that you should just tough it out until the joint is totally destroyed, at which point you simply get a knee replacement. This delay mindset forces you to live with years of unnecessary pain and missed opportunities.
You do not have to accept chronic pain as a normal part of getting older. If you want to know how to stop knee arthritis from progressing and what treatments can keep you out of the operating room, it is time to take action. Explore your non-surgical knee arthritis pain treatment options today, and take the first step toward walking comfortably again.
Leading Manhattan Vascular & Vein Specialist
At Fox Vein Care, we provide state-of-the-art vascular and venous treatments, combining advanced diagnostic technology with minimally invasive procedures that prioritize comfort, safety, and outstanding results.
Contact Us

